
We have evaluated the future health risks associated with fine particulate matter (PM2.5) pollution across Europe under various climate and socio-economic scenarios. We find that PM2.5 remains a leading environmental health risk factor, significantly contributing to chronic diseases and excess mortality despite notable improvements in European air quality in recent decades.
Climate change and socioeconomic scenarios
The study aimed to quantify how future climate change, air pollution, and demographic developments interact to influence health outcomes in Europe. It combined three Shared Socioeconomic Pathways (SSPs)—SSP1-2.6 (sustainability), SSP2-4.5 (middle-of-the-road), and SSP5-8.5 (fossil-fuel intensive)—with climate projections from CMIP6 models. These scenarios represent a wide range of potential futures, from strong mitigation and sustainability to high emissions and limited climate action.
Across all scenarios, PM2.5 levels in Europe are expected to decline significantly in the near term (up to 2040–2050), mainly due to ongoing and planned air pollution control policies. The largest reductions occur under the sustainability pathway (SSP1), where emissions mitigation is relatively strict.
Health impacts
The health burden from PM2.5 exposure, measured as excess mortality, is projected to decrease in the near future across all scenarios due to improved air quality. By 2050, mortality reductions compared to 2010 are estimated at about 55% under SSP1, 43% under SSP2, and 27% under SSP5.
Beyond mid-century, trends diverge significantly. Under SSP1, excess mortality continues to decline and stabilizes at relatively low levels by 2100. Under SSP2, mortality stabilizes or slightly increases. Under SSP5, however, excess mortality rises sharply after 2050, potentially reaching up to 808,000 annual deaths by 2100, roughly doubling current levels.
These differences highlight the strong influence of policy and development pathways on future health outcomes, with up to a fourfold variation in mortality between best- and worst-case scenarios by the end of the century.
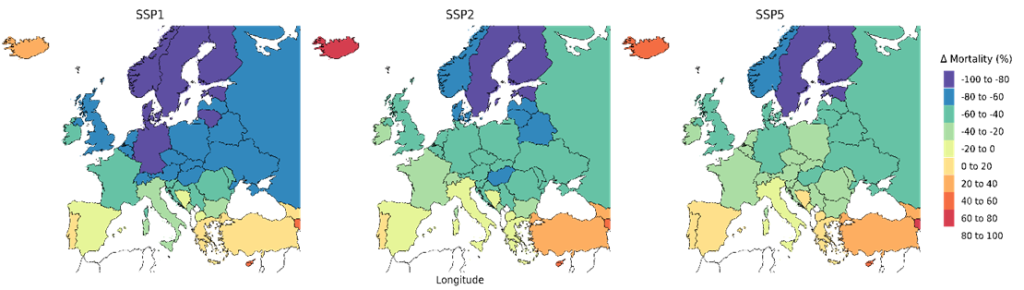
Figure 1: Relative change in population-normalized excess mortality from the exposure to PM2.5 by 2050 compared to 2010, per country and SSP scenario.
Role of demographics
Demographic changes, particularly population ageing and urbanization, play a central role in shaping future health risks. Even as air quality improves, the vulnerability to pollution-related diseases increases in an ageing population. By 2100, the majority of excess mortality is projected to occur in older age groups, especially those over 80 or 90 years old.
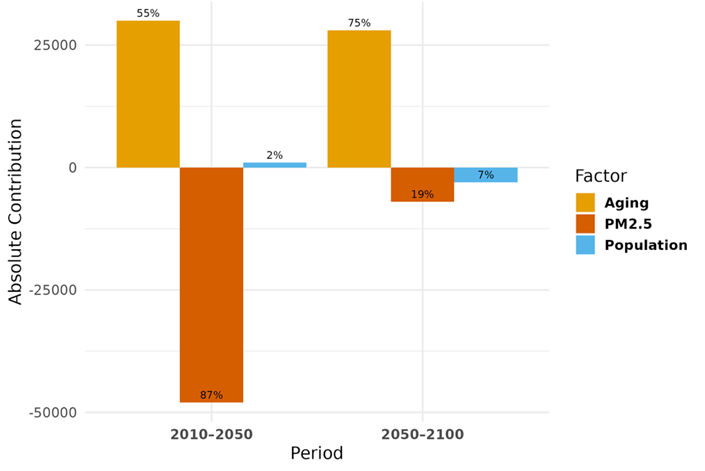
Figure 2: Contribution of population growth, population ageing, and PM2.5 pollution to excess mortality changes between 2010 and 2050, and between 2050 and 2100, under the “middle-of-the-road” SSP2-4.5 scenario.
Population growth and spatial distribution also affect exposure. Urban populations are expected to expand significantly, increasing the number of people exposed to pollution in high-density areas. These trends are most pronounced under SSP5, amplifying health risks despite technological and economic development.
Policy implications
The findings underscore that improvements in air quality alone are insufficient to guarantee reduced health impacts. While emissions reductions are essential, demographic trends and climate-driven changes in pollution dynamics must also be considered.
Key policy implications include:
- Sustained emissions reductions are critical to achieving long-term health benefits.
- Integrated climate and air quality policies are necessary, as climate change can offset gains in pollution control.
- Urban planning and public health strategies must address increasing exposure in growing cities.
- Adaptation measures targeting vulnerable populations, particularly the elderly, are essential.
The study also highlights the importance of aligning with ambitious climate pathways such as SSP1, which combine strong mitigation with sustainable socio-economic development. These pathways, which especially target fossil-fuel-related emissions, offer the most effective means of reducing both pollution levels and associated health burdens.
EU Green Deal: phasing out fossil fuels
The study results suggest that a full phase-out of fossil fuels in the EU27 could yield substantial health benefits. In many countries, exposure to PM2.5 could fall below the strict WHO guideline concentration of 5 µg/m3, nearly eliminating attributable mortality, except in some southern and southeastern European countries (e.g., Italy, Spain, Greece), where additional measures to reduce emissions will be needed. This provides strong support for increasing the share of clean, renewable energy, as advocated by the United Nations through the Sustainable Development Goals for 2030 and the EU’s ambition of climate neutrality for 2050, which is legally binding under the European Climate Law.
Conclusion
The study demonstrates that Europe’s future health burden from air pollution will depend not only on emissions reductions but also on broader socio-economic and climate trajectories. While near-term improvements are likely, long-term outcomes diverge sharply depending on policy choices. Sustainable development pathways can significantly reduce excess mortality, whereas fossil-fuel-driven economic growth may reverse progress and substantially increase health risks.
Ultimately, the results underscore the urgency of coordinated climate, environmental, and public health policies to safeguard population health in a changing climate.
Read the full study: Health risks for Europe and the world of different climate scenarios and the attribution of these risks to sectors (fossil fuel use)
